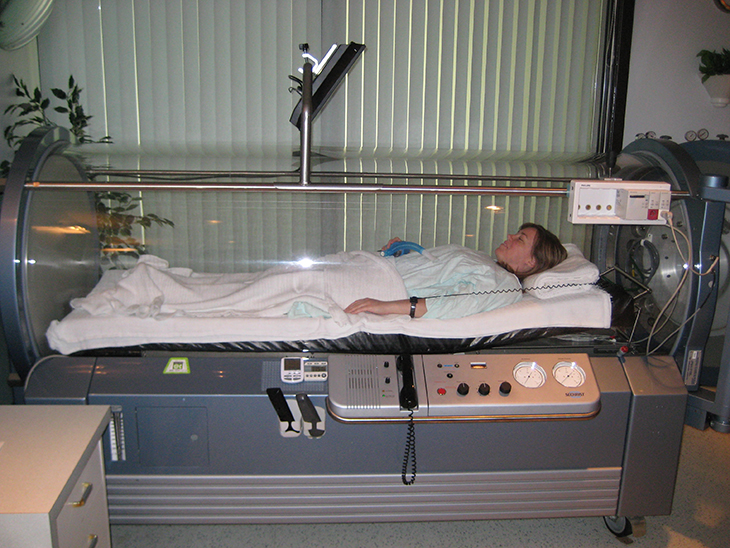
According to a study presented at the Crohn’s & Colitis Congress conference that was held last January 19 to 21 in Denver, Colorado, said that using hyperbaric oxygen treatment (HBOT), a therapy procedure that increases the oxygen supply in the blood to speed up the healing process, could also be used as a safe and effective treatment for those suffering from fistulizing Crohn’s disease. However, the study has yet to be published in the peer-reviewed journal.
When it comes to the HBOT, patients are placed inside a special chamber that creates a pressurized environment and filled with pure oxygen with the intention of filling the blood and repairing the tissues. Moreover, hyperbaric oxygen treatment also encourages the growth of new blood vessels, while working to decrease swelling and inflammation. When inflammation occurs, it can stop the cells from receiving oxygen, hypoxia, which in turn causes tissue to die. Moreover, research shows that hypoxia also induces inflammation, making it a never-ending cycle.
As for gastroenterologist with the Royal College of Physicians UK, Sara Mesilhy, MBBS, “The decreased level of oxygen (hypoxia) and the development of inflammation are described to be two sides of the same coin; they can lead to each other. Inflammatory products increase in cells with low oxygen. Inflamed tissue becomes hypoxic as a result of increases in their metabolic demands.” Notably, Mesilhy was not a part of the study.
Since HBOT has shown to be very effective in treating certain conditions that are related to hypoxia, doctors also found that this type of therapy may be beneficial to those with Crohn’s, which is a well-known type of inflammatory bowel disease, that also have difficult-to-treat and recurrent fistulas.
Because hypoxia also contributes to possible inflammation in those with Crohn’s, it can cause the formation of fistulas as well. These are small tunnels located within the walls of the intestines that can connect to other organs, as well as the skin surface. They tend to cause pain and infection as well. Their presence usually means that inflammation has already penetrated such areas as the skin, organs, or tissue.
Another gastroenterologist at Northwestern Memorial Hospital in Chicago, Parambir S. Dulai, MD, said that “Hyperbaric oxygen therapy is a way to push oxygen into the colon through its tiny blood vessels.” He was referring to another study published in April 2022 where he and his colleagues looked into the benefits of hyperbaric oxygen treatment for those with ulcerative colitis, which is yet another kind of inflammatory bowel disease (IBD).
“This kills the inflammation-causing bad bacteria that thrive in these low-oxygen environments. It resets the immune system and allows the colon to heal,” he said.
For the new study, to have a more extensive understanding of the effectiveness of HBOT on Crohn’s fistulas, an internal medicine specialist with Catholic Medical Center in Manchester, New Hampshire, Amr Dokmak, MD, and other collaborators looked at 16 studies with 164 Crohn’s patients with fistulas that went through 5,125 HBOT sessions.
What they saw in their analysis was that the patients that went through hyperbaric oxygen therapy had an ‘overall clinical response rate of 87 precent.’ In addition, a total of 135 patients out of 164 had a clinical response. Although the definition behind “clinical response” varied from study to study, it still means that generally, there was a substantial improvement overall. One example was a study published in the August 2021 copy of the Journal of Crohn’s and Colitis, which defined clinical response for a patient as “closure of at least 50 percent of fistulas.”
When the research team observed the clinical response for particular types of fistulas, they also saw an 89 percent response for perianal fistulas, or tunnels that develop between the inside of the anus and the outside skin near the anus. In addition, there was an 84 percent response for enterocutaneous fistulas, or abnormal connections that develop between the intestinal tract or stomach, and the skin.
Dr. Mesilhy said, “The response rate mentioned is considered very impressive, making it a promising approach.” UChicagoMedicine explains that advances have been made in the healing of IBD fistula using therapeutics like biologics, which Mesilhy says HBOT could possibly prove to be an efficient addition to the initial or primary therapy.
As for the findings on the perianal fistulas, they were taken from 15 studies that showed that the clinical response in 115 out of 130 patients that were diagnosed with this condition. As for enterocutaneous fistulas, taken from five studies, the clinical response was noted in 21 out of 25 patients.
As for Dr. Dokmak and his team, they found that rectovaginal fistulas – or connections that should not exist between the lower part of the rectum or anus and the vagina – were the fistula subtype that showed the least responsiveness to HBOT, only demonstrating a 29 percent response. They also noted that this response was seen in 4 of 14 cases within five studies.
Meanwhile, the rate of clinical remission – or the closure of fistulas and absence of any type of draining – was seen to be in 59 percent, as based on the gathered data. Remission was seen in 85 out of 143 patients from a total of 14 studies.
As a result, the study authors also concluded that there is a need for randomized control trials in order to validate the benefits that could come with HBOT in fistulizing Crohn’s disease.
Dr. Mesilhy explained, “The beneficial effects of hyperbaric oxygen therapy on inflammatory bowel disease activity may be not only due to increased oxygenation, but also to other changes the therapy makes as it adjusts the immune system by enhancing immune cells that protect the tissue, and enhances genes that produce intestinal barrier–protective elements. The exact long-term effects are still not known, as it varies from one patient to another — further studies are needed to evaluate the long-term effects.”
Treatment Is Usually Expensive
Hyperbaric oxygen therapy has been in existence since 1834, mostly in the treatment of lung – pulmonary – conditions. However, since then, John Hopkins Medicine explains that this type of therapy is mostly used for carbon monoxide poisoning, infections where the tissue is starved for oxygen, gangrene, and wounds that won’t heal.
According to a review published in 2021 in the International Journal of General Medicine, a major drawback of the treatment is its very high cost.
The researchers also explain, “For effective treatment results, there is a need for 20 to 40 sessions of therapy, and one session usually costs $300 in private clinics and about $2,000 in hospitals.”
“There is a need for multiple sessions of therapy, so the treatment may not be affordable for all,” Dr. Mesilhy adds.


