The American Gastroenterological Association has looked into ulcerative colitis and they are now recommending biomarker tests to see if endoscopy is really required for those who have it. Many believe that inflammation levels can now be monitored through certain biomarkers that are present in both the blood and stool.
There are ulcerative colitis patients who no longer need regular monitoring with the use of invasive endoscopies. This was mentioned in the new guidelines released by the American Gastroenterological Association (AGA).
The guidelines were published recently in the journal called Gastroenterology. In it are the highlights that show how biomarker monitoring through noninvasive blood and stool tests are already ample enough for monitoring patients whose ulcerative colitis (UC) is in remission. This can also be true to some with ongoing UC symptoms.
Endoscopies Were Considered to be the Gold Standard for Examining the Body’s GI Tract
Ulcerative colitis is oftentimes the culprit behind the inflammation and sores, or ulcers, in the large intestine. This is why doctors resort to using an endoscope. This is a lighted, flexible tube with a built-in camera on one end. The camera goes into the body to allow the specialist to look into the affected part of the gastrointestinal (GI) tract.
There are two types of endoscopies for testing ulcerative colitis. This was per the Crohn’s & Colitis Foundation. A sigmoidoscopy allows the doctor to examine the inflammation in the lower colon and rectum. A total colonoscopy, on the other hand, examines the whole colon.
The endoscopy is a procedure that’s considered to be the gold standard for examining and monitoring ulcerative colitis and seeing if there’s bowel inflammation. However, the authors behind the new guidelines set that this is also invasive, expensive, and more importantly, often requires weeks of waiting just to schedule.
“Fecal and blood testing, however, can [provide] objective evidence about inflammation, worsening inflammation, and improved inflammation without having to necessarily subject the patient to invasive procedures, such as colonoscopy or similar insertion of a scope into an orifice of the body,” explained gastroenterologist Russell Cohen, MD. He is the director of the UChicago Medicine Inflammatory Bowel Disease Center. He also was not part of the group of authors who wrote the new guidelines. These tests can already see if the medicines are effective and if the disease is under proper management.
Biomarkers Used for Monitoring Ulcerative Colitis
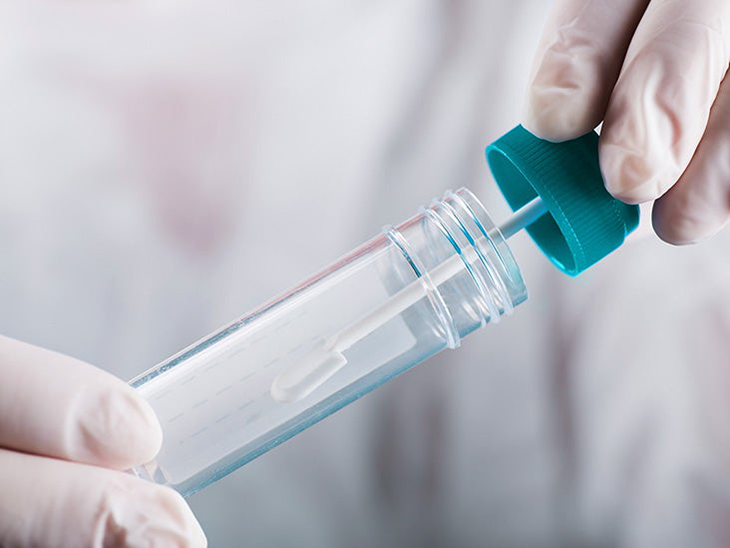
The AGA recommendations set hone in on three specific biomarkers that can provide doctors with a precise look into the ulcerative colitis disease activity: fecal calprotectin and fecal lactoferrin, which can be detected in stool, and serum C-reactive protein (CRP), which can be seen in blood.
The new guidelines suggest that biomarker testing need to actually be the primary step when it comes to determining if there’s a need for endoscopic testing for those who suffer from symptomatic UC. They also advise patients to get biomarker monitoring every 6 to 12 months in UC patients who are considered to be in symptomatic remission.
As for the new tests, stool tests are said to be better than its blood counterpart, according to the authors. They say that this is favored because stools are more sensitive. The doctors will be able to detect even mild inflammations. More importantly, these are said to also be more specific because the measurements would be elevated only from intestinal inflammation instead of any incidental ongoing medical issues like respiratory infections.
When Endoscopy is Not Needed
For those who are in symptomatic remission and who have normal biomarkers, the AGA said that they also need to continue their biomarker monitoring activities but also need to stay away from routine endoscopic assessments.
The guidelines say that endoscopic assessments should be avoided for those diagnosed with moderate to severe symptoms and elevated biomarkers.
“If there are severe symptoms and elevated biomarkers, this confirms the symptoms are from active ulcerative colitis,” said Ashwin N. Ananthakrishnan, MBBS, MPH. He is the guideline author as well as a gastroenterologist with Massachusetts General Hospital in Boston. “One does not need to wait for an endoscopy in this setting and should initiate treatment early without delay.”
Endoscopy is Still Required for Some Cases
The AGA said that endoscopic assessments are still required in the following cases:
- Symptomatic remission that come with elevated biomarkers
- Mild symptoms that come with normal or elevated biomarkers
- Moderate to severe symptoms that come with normal biomarkers
“Biomarkers are imperfect, and some patients, despite significant inflammation, may not have a rise in biomarkers,” also added guidelines author Siddharth Singh, MD. He is a gastroenterologist with the University of California in San Diego. “In these situations, endoscopy can help gauge inflammation and also help evaluate potential other causes of symptoms, like specific infections.”
Dr. Ananthakrishnan also have his opinion and said that endoscopy is helpful when it comes to seeing the appropriate level of treatment that the patient requires.
“If the symptoms are not from the underlying UC, there is risk of inappropriate overtreatment,” he says. “On the other hand, if the biomarker is falsely normal, there is risk of inappropriate undertreatment. That’s why an endoscopic assessment is needed.”
Basically, it will still be up to the physician if endoscopy is required, Dr. Cohen said.
“There are cases where I see the data but I still want to look with the scope, and that should be allowed — it’s really up to the judgment of the doctor,” he explained.
While the AGA said that a monitoring strategy must include biomarkers and symptoms instead of just looking at the symptoms, they also come to the conclusion that more evidence was required before they will fully recommend a biomarker-based monitoring strategy instead of a endoscopy-based monitoring method.
For Further Insurance Coverage
When it comes the costs and payment of these biomarker tests, there is a big difference in coverage across different healthcare plans, the guideline authors also added.
“Stool tests are sometimes not covered by insurance and deemed to be ‘experimental’ despite extensive data,” said Dr. Singh. “Through these guidelines, we hope to change that so that these tests are routinely covered by insurance. That will be a win for patients, providers, and our overburdened healthcare system.”